Are primary and secondary insurance billed at the same time?
It is a common mistake to think that primary and secondary insurance claims get billed out at the same time. However, this is incorrect. When billing for primary and secondary claims, the primary claim is sent before the secondary claim.
How does primary and secondary insurance get billed?
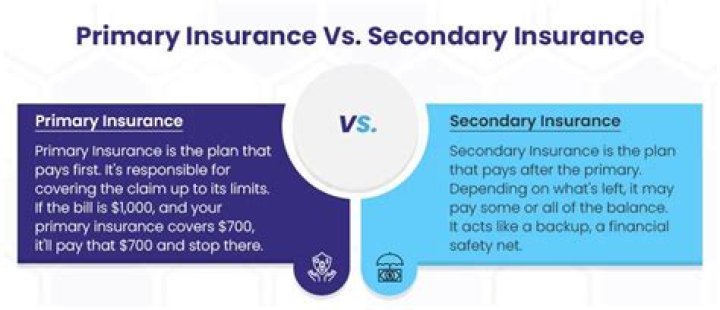
Primary insurance pays first for your medical bills. Secondary insurance pays after your primary insurance. Usually, secondary insurance pays some or all of the costs left after the primary insurer has paid (e.g., deductibles, copayments, coinsurances).
What are primary and secondary payers in medical billing?
A primary payer is the insurer that pays a healthcare bill first. A secondary payer covers remaining costs, such as coinsurances or copayments.
How does primary and secondary insurance work with deductibles?
What does primary and secondary insurance mean? Primary insurance pays first up to coverage limits. Then secondary insurance pays if there is a balance that the primary insurance didn’t cover. However, even with primary and secondary insurance, you may not have 100% of your costs, such as deductibles, covered.
What is the process of determining which company is primary and which is secondary?
This process is called coordination of benefits. Coordination of benefits decides which plan pays first (the primary plan) and which pays second (the secondary plan).
How do you determine which insurance is primary?
Primary coverage generally comes from the plan that belongs to the parent whose birthday comes first in the year. So if one parent’s birthday is February 6 and the other’s is October 3, the kids will have primary coverage from the parent whose birthday is in February.
When to create a secondary claim in simplepractice?
Within SimplePractice, you’re only able to create a secondary claim after you’ve successfully created a primary claim. The Create Secondary Claim button won’t appear on the primary claim unless the client has a secondary insurance on file and until the primary claim is in any of the statuses below:
When does the create secondary claim button appear?
The Create Secondary Claim button won’t appear on the primary claim unless the client has a secondary insurance on file and until the primary claim is in any of the statuses below: If your primary claim is in one of the above statuses, you’ll see the Create Secondary Claim button appear on the primary claim:
Do you pay first to primary or secondary insurer?
You don’t get to choose which insurer will pay a certain claim. However, if the first insurer doesn’t cover a certain treatment, or covers it only partially, you can then submit the remainder of the claim to your secondary insurer for payment, assuming the treatment is covered under the second plan. So who pays first?
How do I make a secondary insurance claim?
If your primary claim is in one of the above statuses, you’ll see the Create Secondary Claim button appear on the primary claim: By clicking the Create Secondary Claim button, a new secondary claim will be generated with the client’s secondary insurance information populated on the claim form.