What does in network mean in health insurance?
What is In-Network? When you see a doctor who is in-network, you are using a provider who participates in one of CareFirst’s provider networks. Some health insurance plans only cover care in-network, while other health plans cover both in-network and out-of-network care.
What does medical providers in network mean?
A provider network is a list of health-care providers who are contracted by an insurance company, and provide medical care to those enrolled in plans offered by that insurance company. The providers in the health insurance plan’s network are called “network providers” or “in-network providers”.
How do I know what is in network for my insurance?
How to Verify In-Network Providers
- Check your insurance company’s website. Many insurance companies will post in-network providers for the plans they offer.
- Check your provider’s website.
- Call your provider.
- Call your insurance company.
- Call your agent.
Is in network cheaper than out of network?
How does it impact out-of-pocket expenses? Obtaining health care services from a healthcare professional or facility that is in-network is generally (much) cheaper than out-of-network.
What is in network and out of network in medical billing?
When a doctor, hospital or other provider accepts your health insurance plan we say they’re in network. We also call them participating providers. When you go to a doctor or provider who doesn’t take your plan, we say they’re out of network.
What insurance requires a doctor to use in the insurance company network?
Health Maintenance Organizations (HMOs) You must use providers in the HMO network. Usually, you must have a primary care doctor. This doctor provides your basic care and coordinates referrals to specialists.
Why do health insurance companies use provider networks?
Provider networks enable health plans to make care more affordable for consumers by negotiating better prices with physicians and hospitals in the network.
How do I know what doctors are in my network?
Call your doctor’s office and ask for your doctor’s specific tax ID number. Call your insurance carrier at their general line and give them the specific name of your plan and your doctor’s tax ID number. They’ll be able to tell you whether or not your doctor is in-network.
In network refers to providers or health care facilities that are part of a health plan’s network of providers with which it has negotiated a discount. Insured individuals usually pay less when using an in-network provider, because those networks provide services at lower cost to the insurance companies…
What happens when you use an out of network provider?
If you use an out-of-network provider, health care services could cost more since the provider doesn’t have a pre-negotiated rate with your health plan. Or, depending on your health plan, the health care services may not be covered at all.
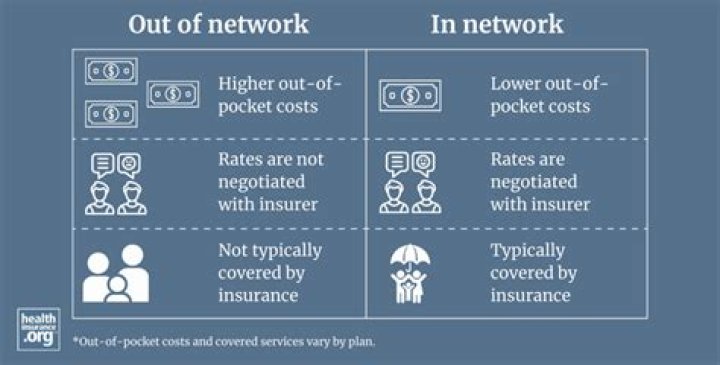
What does in network and out of network mean?
In-network refers to a health care provider that has a contract with your health insurance plan to provide health care services to its plan members at a pre-negotiated rate. Because of this relationship, you pay a lower cost-sharing when you receive services from an in-network doctor. What does out-of-network mean?
What do you mean by provider in health insurance?
Provider —any person (i.e., doctor, nurse, dentist) or institution (i.e., hospital or clinic) that provides medical care. Rider —coverage options that enable you to expand your basic insurance plan for an additional premium.