What does secondary insurance coverage mean?
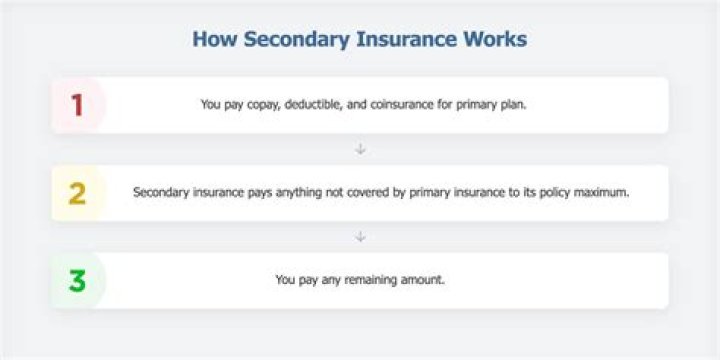
Secondary health insurance is coverage you can buy separately from a medical plan. It helps cover you for care and services that your primary medical plan may not. These are also called voluntary or supplemental insurance plans. Some secondary insurance plans may pay you cash.
What is the difference between primary and secondary health insurance?
Primary insurance: the insurance that pays first is your “primary” insurance, and this plan will pay up to coverage limits. You may owe cost sharing. Secondary insurance: once your primary insurance has paid its share, the remaining bill goes to your “secondary” insurance, if you have more than one health plan.
Will secondary insurance pay if Medicare denies?
Secondary insurance pays after your primary insurance. If your primary insurance denies coverage, secondary insurance may or may not pay some part of the cost, depending on the insurance. If you do not have primary insurance, your secondary insurance may make little or no payment for your health care costs.
What does secondary insurance mean in health insurance?
Secondary insurance is coverage that is available in addition to a primary health insurance plan and covers gaps in traditional health insurance coverage.
Can you buy secondary insurance through your employer?
If you buy a medical plan on your own through the Health Insurance Marketplace, you can purchase supplemental or secondary coverage through a private insurance company. If you get your medical plan through your employer, you may have the option to add one or more secondary or supplemental plans during enrollment.
Do you pay first to primary or secondary insurer?
You don’t get to choose which insurer will pay a certain claim. However, if the first insurer doesn’t cover a certain treatment, or covers it only partially, you can then submit the remainder of the claim to your secondary insurer for payment, assuming the treatment is covered under the second plan. So who pays first?
Can you get secondary health insurance for a high deductible?
Can you get secondary health insurance to cover a high deductible, a copay, or coinsurance? Yes, you can get secondary medical insurance to help cover out-of-pocket costs. This may include a deductible, your copays, and coinsurance payments. This type of plan is often called a “limited benefits” plan or simply “gap insurance.”