What is the key difference between traditional indemnity insurance and managed care?
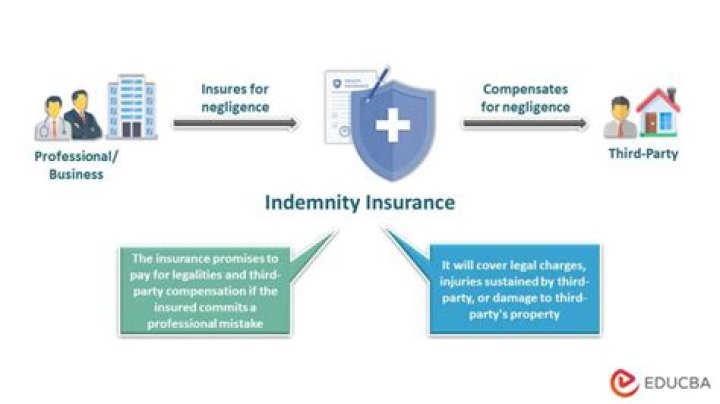
What are some key differences between traditional indemnity insurance and managed care? Indemnity insurance plan allows the insured to obtain health care services anywhere and from any physician or hospital. Tradition insurance: -no incentive to managed delivery of health services and how the providers got paid.
What are three ways that a managed care plan differ?
There are three types of managed care plans:
- Health Maintenance Organizations (HMO) usually only pay for care within the network.
- Preferred Provider Organizations (PPO) usually pay more if you get care within the network.
- Point of Service (POS) plans let you choose between an HMO or a PPO each time you need care.
What is managed care insurance plan?
Managed care plans are health insurance plans with the goal of managing two major aspects of healthcare: cost and quality. With these plans, the insurer signs contracts with certain health care providers and facilities to provide care for their members at a reduced cost.
What are some of the key differences between traditional managed care and accountable care organizations?
The MCO is a group of medical providers and facilities that provide care to its members at a reduced cost. Many MCO’s require the patient to have a primary care provider. The ACO is a group of medical providers and medical facilities that work together to provider collaborative care to its members.
What are the four most common types of managed care plans?
Different Types of Managed Healthcare Plans: HMO, PPO, POS, EPO Explained
- Health Maintenance Organization (HMO)
- Preferred Provider Organization (PPO)
- Point of Service Plan (POS)
- Exclusive Provider Organization (EPO)
What are the two major difference between managed care and indemnity insurance?
Indemnity plans do give you more freedom, however, than managed care plans in terms of using the healthcare provider of your choosing. So, as with anything else, the choice between managed care and indemnity plans ultimately depends on your personal circumstances and preferences.
What is an example of a managed care plan?
A good example of a managed care plan is an HMO (Health Maintenance Organization). HMOs closely manage your care. Your cost is lowest with an HMO. You are limited to seeing providers in a small local network, which also helps keep costs low.
What are the six models of managed care?
Terms in this set (6)
- IDS (Intregrated Delivery System. Affiliated provider sites that offer joint healthcare.
- EPO (Exclusive Provider Organization.
- PPO ( Preferred Provider Organization)
- HMO (Health Maintence Organization)
- POS (Point of Sale)
- TOP (Triple Option Plan)
Who is eligible for managed care plans?
While about 90 percent of Medicaid beneficiaries are enrolled in some form of managed care, the proportion of beneficiaries enrolled in managed care, the rate of enrollment growth, and spending on managed care varies among the major Medicaid eligibility groups (non-disabled children and adults, individuals with …
What is a managed care organization example?
Managed care organization examples include: Independent Physician or Practice Associations. Integrated Delivery Organizations. Physician Practice Management Companies.
What’s the difference between managed care and traditional health insurance?
Define Indemnity Health Insurance. Managed care health insurance plans and traditional medical insurance plans differ widely from each other. Two common types of managed care plans are preferred provider organizations, also called PPOs and health maintenance organization, also known as HMOs.
What are the different types of managed care plans?
Two common types of managed care plans are preferred provider organizations, also called PPOs and health maintenance organization, also known as HMOs. In terms of use, traditional plans usually give the subscriber greatest flexibility and cost the most.
What are the advantages of a managed health care plan?
Advantages of Managed Health Care Plans: HMO, PPO, or POS The managed health care plan proposition provides benefits to both plan members and sponsors. Managed health care plan members benefit from reduced rates and guaranteed access to health care services Members of the health network benefit from having a steady stream of clients
What’s the difference between fee for service and managed care?
There is no state boundary under fee-for service, you can go for any hospital or clinics in any state in the U.S. The insurer will pay up to 80% of any medical bills, if you reach the yearly deductible. The insurer will pay 100% medical expenses, if you reach the out-of-pocket maximum. Fee-for-service requires higher premiums and more paper work.