Why is my EPO more expensive than PPO?
Since you do have a restriction of using an exclusive network with the EPO plan, it is often cheaper than a PPO plan, making it an excellent compromise for those looking to have more control over their healthcare without paying significantly more in insurance premiums.
Do EPO plans have out of network benefits?
EPO stands for “Exclusive Provider Organization” plan. As a member of an EPO, you can use the doctors and hospitals within the EPO network, but cannot go outside the network for care. There are no out-of-network benefits.
How does EPO insurance work?
An EPO, or Exclusive Provider Organization, is a type of health plan that offers a local network of doctors and hospitals for you to choose from. If you’re looking for lower monthly premiums and are willing to pay a higher deductible when you need health care, you may want to consider an EPO plan.
Do EPO plans require referrals?
You do not need a referral to see a specialist with an EPO. This can make it easier to get the care you need, whenever you need it. At the same time, make sure to visit a specialist who is in your network, because your insurance company may leave you with the bill if you go out of network.
Does an EPO have a deductible?
The deductible is a specified annual dollar amount you must pay for covered medical services before the plan begins to pay benefits. EPO deductibles are flat amounts, as shown on the Key Provisions chart.
What does EPO do to your body?
EPO helps make red blood cells. Having more red blood cells raises your hemoglobin levels. Hemoglobin is the protein in red blood cells that helps blood carry oxygen throughout the body. Anemia is a disorder that occurs when there is not enough hemoglobin in a person’s blood.
Why EPO is dangerous?
It is well known that EPO, by thickening the blood, leads to an increased risk of several deadly diseases, such as heart disease, stroke, and cerebral or pulmonary embolism. The misuse of recombinant human EPO may also lead to autoimmune diseases with serious health consequences.
What does an EPO cover?
An exclusive provider organization, or EPO, is a health insurance plan that only allows you to get health care services from doctors, hospitals, and other care providers who are within your network. Your insurance will not cover any costs you get from going to someone outside of that network.
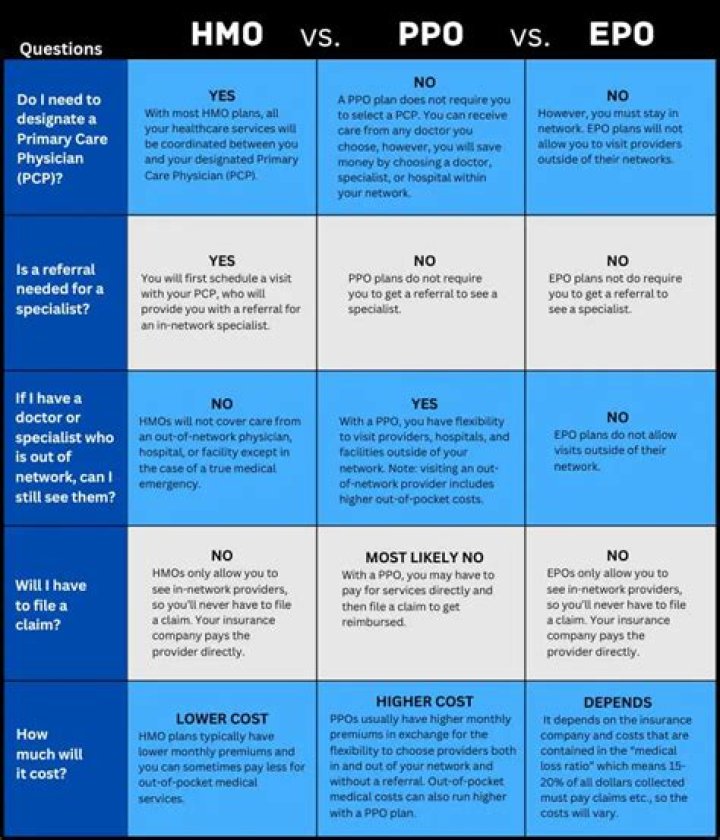
What’s the difference between a PPO, EPO, and POS?
HMOs, PPOs, EPOs, and POS plans all have provider networks. This network includes doctors, hospitals, labs, and other providers that either have a contract with the health plan or, in some cases, are employed by the health plan. Plans differ as to whether you’ll have coverage for health care services from providers who aren’t in their network.
Can a health insurance plan pay for an EPO?
Apart from in exceptional circumstances, such as emergency care, an EPO will not pay anything toward treatment undertaken with healthcare providers from outside its network. Restrictions imposed by various types of health insurance plans – HMO, PPO, POS and EPO.
Which is better an exclusive provider organization or PPO?
An Exclusive Provider Organization, or EPO, is a type of health insurance plan in which members must utilize doctors and providers within the EPO network, except in case of a medical emergency. One of the most significant advantages to an EPO is participants don’t need a referral from a primary care physician to see a specialist.
What’s the difference between HMO and PPO health insurance?
HSA stands for health savings account, and HSA-qualified plans can be HMOs, PPOs, EPOs, or POS plans. HSA-qualified plans must meet specific plan design requirements laid out by the IRS, but they are not restricted in terms of the type of managed care they use.